Oral Surgery: What is it and how do I know when I need it?
What is oral surgery?
Oral surgery is a specialty of dentistry focusing on the health of your head, neck, and jaws. There are several common dental procedures that involve oral surgery, including tooth extractions, root canal therapy, dental implants, and much more. Depending on your specific needs, your dental professional may refer you to an oral maxillofacial surgeon.
What to expect during your oral surgery?
Oral surgery can sound intimidating, but don’t worry, your dental professionals are here to guide you through the entire process. You will initially have a consultation to discuss your specific diagnosis and treatment needs, as well as answer any questions or concerns you may have. Your medical and dental history will be reviewed, and you will be informed of what your procedure entails along with any potential risks involved.
Signs that you need oral surgery
Feel like something’s off in your oral cavity? If you notice you’re having any issues with your teeth, gums, or jaws, it is important to talk with your dentist as soon as possible. After a thorough exam, your dentist will determine if you may need oral surgery and will refer you to the right professional.
Impacted wisdom tooth extraction
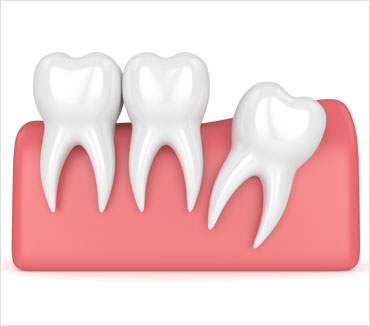
Wisdom teeth, also known as third molars, are the last teeth to erupt into the mouth. Yet, in many individuals there is often not enough space for these teeth to erupt naturally, causing them to become impacted. Impacted wisdom teeth fail to poke fully through the gums and are trapped within the jawbone. This can be totally asymptomatic or cause annoying pain. In addition, impacted wisdom teeth may even cause damage to other teeth or lead to swelling and infection. In these cases, impacted wisdom teeth are often recommended by a dental professional to be removed. Once an impacted wisdom tooth is removed, stitches are often used to close the extraction site and let the gums heal. Your dentist will explain all post-surgical instructions that are necessary to follow.
Jaw Alignment Surgery
Jaw alignment surgery may be recommended for individuals who have a misaligned bite. This could be due to abnormal growth of the jaws or a result of an injury. Jaw surgery often requires a dental team, including oral maxillofacial surgeons, orthodontists, and other dental specialties. Treatment may involve your upper jaw, lower jaw, or both. Jaw surgery is often not recommended until an individual is done growing, which can sometimes be around the mid-’20s. As with all surgical procedures, your dental professionals will inform you of all risks, benefits, and alternative treatment options associated with the procedure needed.
Temporomandibular Joint Disorders
Temporomandibular joint disorders can be a real pain, literally. The temporomandibular joint (TMJ), located on each side of your jaw, helps control jaw movement. If damaged, your dental professional may recommend TMJ surgery, which can include arthrocentesis, arthroscopy, or open joint surgery. Arthrocentesis involves the injection of fluids into the joints to help eliminate any inflammatory debris. Arthroscopy involves the insertion of a thin tube to help diagnose and treat the joint. If more severe, open joint surgery may be recommended to expose and repair the joint.
Tooth Loss
Tooth loss negatively impacts your smile and oral health. Plus, chewing and speaking can become difficult when teeth are lost. It can be a result of many factors, such as gum disease, trauma, or tooth decay. When teeth are lost, the surrounding bone also starts to resorb and break down. Fortunately, replacing missing teeth with prosthetic restorations can help prevent bone loss from occurring. Common treatment options include bridges, dentures, and dental implants. If you are looking to replace missing teeth, your dental professionals can help you make the best treatment decision.
Tooth Extraction
For tooth extraction, your dentist will numb the area with local anesthesia so that you won’t feel pain throughout the procedure. Bleeding is a common occurrence after the procedure, but will soon resolve once a blood clot forms at the extraction site. Instructions will be given following the procedure, including avoiding the use of straw or smoking. Your dental professional will recommend which pain medications to consume depending on the procedure and your medical history.
Sleep Apnea Treatment
Sleep is an important part of our daily lives. Sleep apnea has been linked to many oral and overall health problems, including diabetes, heart disease, and obesity. Sleep apnea occurs when breathing temporarily stops and starts during sleep. When diagnosed, your dental professional may suggest treatment to open your airways, such as a continuous positive airway pressure (CPAP) machine, a bi-level positive airway pressure (BiPAP) machine, an adaptive servo-ventilation machine (ASV), or oral appliances such as night guards that advance the lower jaw forward. Lifestyle changes including weight loss, repositioning the way you sleep and avoiding alcohol before bedtime have also been linked to improving mild cases of sleep apnea. If sleep apnea cannot be managed by these treatment options, surgery is often indicated. One of the most common surgeries to treat sleep apnea is an uvulopalatopharyngoplasty (UPPP), which removes extra tissue from the soft palate and pharynx to allow for better breathing. Other surgeries may involve jaws or nasal structures.
Root Canal Therapy
A root canal is often recommended once dental pulp, the innermost layer of the tooth, becomes infected. The pulp contains an abundance of nerves, connective tissue, and blood vessels necessary to keep the tooth alive. Once infected, you may experience pain, swelling, and sensitivity when consuming hot or cold foods. To confirm infection within the pulp, a dental x-ray will be taken and examined by your dentist. Common causes of pulpal damage include tooth decay, a fractured tooth, and/or injury to the tooth. Root canal therapy involves numbing the affected tooth with local anesthesia and accessing the tooth’s root canal by creating an opening at the top of the tooth. Once accessed, your dentist will remove the infected pulp tissue with special files. Once the canals of your root are cleaned, your dentist will fill the tooth with a material called gutta-percha. Once the canal is filled, the top opening of your tooth will be filled with a temporary filling. Your dental professional will then instruct you on any additional needed procedures following the root canal to ensure the health of the tooth.
Oral Cancer
Oral cancer is often treated with surgery. Depending on the location and stage, there are several surgical options that may be recommended. Oral cancer screenings are performed at each dental visit and can be managed more efficiently when caught early.
What to eat after oral surgery
After an oral surgery procedure, soft foods at room temperature are typically recommended. You will often be instructed to avoid smoking, consuming hard or chewy foods, or using a straw to allow for proper healing. For some procedures, you may be advised to arrange to have someone pick you up from your appointment to drive you home.
What to expect during recovery
Following a surgical procedure, recovery is an important stage. It will be important to avoid smoking or consuming alcohol, as these habits may slow your healing process. It may be recommended to perform salt water rinses every few hours at home to help promote healing. If you notice any irregular symptoms lasting longer than anticipated as determined by your dental professional, be sure to contact them immediately.
Our doctors and dental specialists provide a wide range of dental services at our 40+ multi-specialty dental offices across Massachusetts and New Hampshire. Our dental team is compassionate, and our main goal is to provide you a comfortable, caring dental experience. Book an appointment at your local Gentle Dental today.



